Cerebral Palsy, the symptoms.
Some figures about Cerebral Palsy (CP):
- 17 million people in the world have cerebral palsy (i.e. 125,000 persons in France)
- 1 in 400 to 500 babies is born with Cerebral Palsy (that’s 1500 new cases a year in France)
- 1 person out of 3 is unable to walk
- 1 out of 2 people with CP lives with chronic pain
- 1 out of 5 people with CP is unable to speak
- 1 out of 10 people with CP has severe vision impairments
- 1 out of 25 people with CP has severe hearing impairments
- 40% of affected people were born prematurely.
In France, this pathology is also known as “Infirmité Motrice Cérébrale (IMC)”, meaning Cerebral Movement Disability. Cerebral palsy is an umbrella term that refers to a group of disorders affecting the posture and movement coordination of a person. It is due to the destruction of certain types of cells which occurred in the developing brain during pregnancy or shortly after birth (before 2 years old). Thus, the brain does not send the correct orders to muscles.
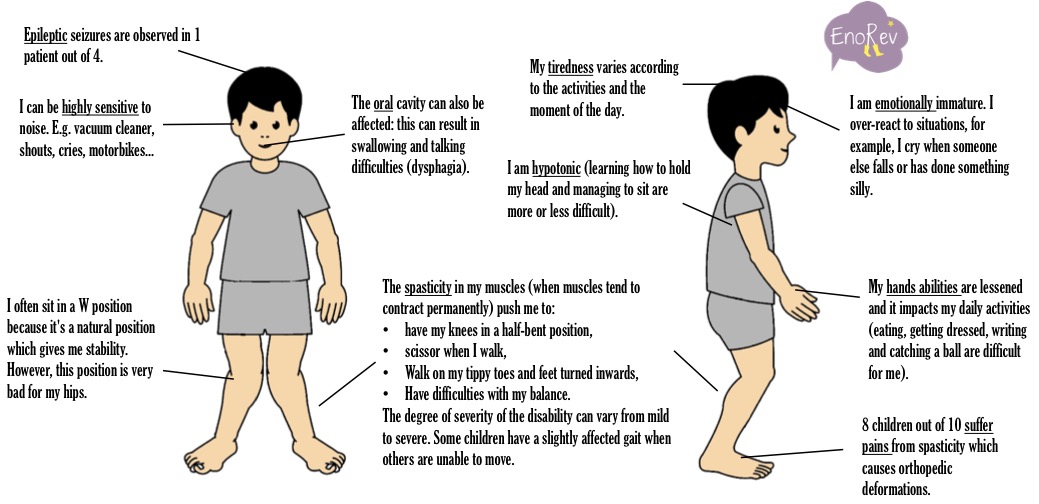
The movement disorders of Cerebral Palsy can also come with a range of associated physical and cognitive issues: sense, perception, cognitive, communication and behaviour impairments, epileptic seizures and secondary bone-muscles disorders. You will find all the symptoms on the drawing below. The symptoms may have different degrees of severity:
The pathology can affect people in different ways and with different intensity. The three main forms are:
- spastic diplegia, also known as Little’s Syndrom, when the the lower limbs are affected (Enora A’s case),
- spastic quadriplegia, when the four limbs are affected (Enora T’s case),
- spastic hemiplegia, when the arm and the leg of one side of the body are affected.
In practice, we observe muscles disorders: depending on where the damage is in the brain, some muscles can be permanently too tight, or not tight enough, or alternate uncontrollably between these two states. The main symptom is spasticity : it is a muscular phenomenon which defines the tendency of a muscle to be permanently contracted. When the person wants to do a movement, antagonistic muscles simultaneously get the order to contract.As a consequence, the typical posture and gait are as follow:
- knees in a half-bent position as well as a crouched posture because the muscles in charge of flexions are more powerful than those for stretching,
- scissors-like gait: the tension of the hips muscles force the knees on the inside,
- feet stretched on their toes (bilateral equinus) and turned inwards (varus).
There are also muscular weaknesses due to a lack of use of certain muscles.
Another characteristic of Cerebral Palsy is the reflex anomalies (automatic reactions). For example:
- Despite the diversity of clinical cases, 100% of children who have CP have unusual anti-gravitation reactions which cause a lack of postural adaptation and a difficulty in balance management.
- In most children with CP, there is no opposite weight transfer when one limb is lifted, which explains why it’s difficult for them to crawl, walk on all four, stand up, etc… This deficiency can be more or less countered acted by voluntary movements.
These adaptation disorders are worsened by a proprioception deficiency. . This is the ability to perceive oneself, consciously or not, that is to say the position of the various limbs and of their tone in relation to the situation of the body in space.
It is often said that it is a non-progressive disability. Yet, the damaged part of the brain remains permanently damaged and does not develop throughout the life of the person, and the growth of the child does in fact make the management of this disability ever evolving. Indeed, the constant contraction of muscles causes bone distortion as the child grows. As the muscle is less solicited, soft tissue retractions appear and the biomechanical quality of joints deteriorates. It is therefore a vicious circle, you have to fight to avoid, when possible, orthopaedic deformations and the development of bad posture. For example, adductor muscles are often spastic, which often leads to hip displacement or dislocation. The evolution of hip displacement is fastened by the W position the child automatically takes when sitting (between heels) in order to stabilize her/his position when playing on the floor.